Are injectable contraceptives suitable for you? Dr. Purnima Badve helps you weigh the pros and cons, so you can make an informed decision. Injectable contraceptives are used as a temporary method of contraception by females. They have been in use in India since 1992. They are widely accepted in USA, Europe and parts of Asia, especially in Thailand and Indonesia. Injectable Contraceptives (ICs) are made up of progestational compounds. Progesterone is one of the female sex hormones. This hormone is normally present in healthy, adult women during the latter half of their menstrual cycle. In this articleMode of AdministrationContraceptive BenefitsOther non-contraceptive benefitsDISADVANTAGESThere are 2 types of ICs available in the market. They are: Noristerat (Chemical name - Norethindrone Enanthate, also called Net-en) Noristert is to be given every 2 months. Depo Provera (Chemical name - Medroxyprogesterone acetate) Depo Provera is to be given every 3 months. Both are available as single dose ampules. Either of the two can be used. The choice is yours or your gynaecs! Mode of Administration Deep intra-muscular injection, preferably gluteally, with usual the antiseptic precautions. This injection is NOT to be massaged. However, you could apply light pressure to the injected area for 1-2 minutes. The first IC injection is to be given: a) Between the 1st and 5th days of the menstrual cycle. It can be given during or immediately after the menstrual period. b) Anytime during the menstrual cycle, if the woman and her doctor are sure that she is not pregnant. c) Postpartum - 6 weeks after normal delivery or Caesarian delivery. d) Post abortion - immediately or within 7 days after abortion. The second injection should be taken exactly after 2 months in case of Noristert, and after 3 months in case of Depo Provera. Upto 4 days earlier or upto 4 days later than the stipulated date is permissible. ICs can be given in most cases where Estrogen containing oral pills are contraindicated or not tolerated. ADVANTAGES A. Contraceptive Benefits They have a 99% rate of efficacy during the first year of use, and are thus very effective. Their effect is rapid. They start working within 24 hours after administration. A pelvic examination is not required prior to use. They do not interfere with intercourse. They do not affect breast-feeding. They can be given to lactating women without any effect on the baby or on the amount of breast milk. They have minimal side effects. There is no nausea, rise in blood pressure or any clotting disorder associated with their use. In fact, these risks are associated with oral pills. However, cases of mild headaches or dizziness should be reported to the doctor. They provide you with protection for 2 to 3 months. There is no need to use any other form of contraception during this period. B. Other non-contraceptive benefits May decrease menstrual cramps. May decrease menstrual bleeding. May improve anemia. Protects against some causes of pelvic inflammatory diseases. Decreases chances of ectopic pregnancy. Decreases benign breast disease. Protects against endometrial cancer. Any nurse or trained non-medical staff can administer the injection. There is no need to book an appointment with your gynaec every time you need a shot. DISADVANTAGES Menstrual Irregularities - Spotting, breakthrough bleeding and sometimes skipping of your periods are the side effects of these contraceptives. However, skipping of your periods is natural when you are on the IC and it does not cause any harm… and, of course, it helps in cases of anemia! Planning or postponement of the period is not possible when the woman is on ICs. One cannot accurately predict the timing of the period, which may create a slight problem, especially when planning a holiday or even religious function. There may be a delay in return to fertility after discontinuing ICs. Pregnancy may not occur immediately. On an average it takes 2-3 months after you stop taking the pill or removing a Copper T to resume fertility. If you are using injectable contraception, this period is longer, and can be 4 to 5 months. ICs do not provide protection against STDs or HIV. Neither do oral pills for that matter. Only condoms or any other barrier method of contraception can provide this protection.
Are injectable contraceptives suitable for you? Dr. Purnima Badve helps you weigh the pros and cons, so you can make an informed decision.
Injectable contraceptives are used as a temporary method of contraception by females. They have been in use in India since 1992.
They are widely accepted in USA, Europe and parts of Asia, especially in Thailand and Indonesia.
Injectable Contraceptives (ICs) are made up of progestational compounds. Progesterone is one of the female sex hormones. This hormone is normally present in healthy, adult women during the latter half of their menstrual cycle.
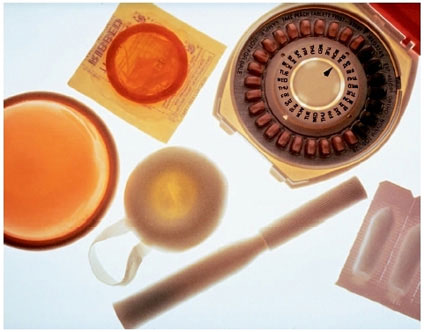
There are 2 types of ICs available in the market. They are:
- Noristerat (Chemical name - Norethindrone Enanthate, also called Net-en) Noristert is to be given every 2 months.
- Depo Provera (Chemical name - Medroxyprogesterone acetate) Depo Provera is to be given every 3 months.
Both are available as single dose ampules. Either of the two can be used. The choice is yours or your gynaec's!
Mode of Administration
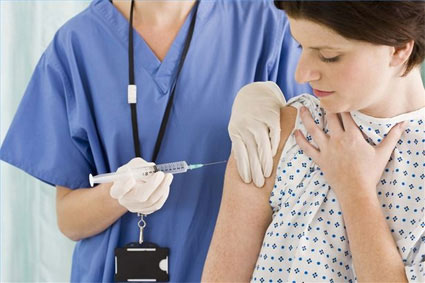
Deep intra-muscular injection, preferably gluteally, with usual the antiseptic precautions.
This injection is NOT to be massaged. However, you could apply light pressure to the injected area for 1-2 minutes.
The first IC injection is to be given:
a) Between the 1st and 5th days of the menstrual cycle. It can be given during or immediately after the menstrual period.
b) Anytime during the menstrual cycle, if the woman and her doctor are sure that she is not pregnant.
c) Postpartum - 6 weeks after normal delivery or Caesarian delivery.
d) Post abortion - immediately or within 7 days after abortion.
The second injection should be taken exactly after 2 months in case of Noristert, and after 3 months in case of Depo Provera. Upto 4 days earlier or upto 4 days later than the stipulated date is permissible.
ICs can be given in most cases where Estrogen containing oral pills are contraindicated or not tolerated.
ADVANTAGES
A. Contraceptive Benefits
- They have a 99% rate of efficacy during the first year of use, and are thus very effective.
- Their effect is rapid. They start working within 24 hours after administration.
- A pelvic examination is not required prior to use.
- They do not interfere with intercourse.
- They do not affect breast-feeding. They can be given to lactating women without any effect on the baby or on the amount of breast milk.
- They have minimal side effects. There is no nausea, rise in blood pressure or any clotting disorder associated with their use. In fact, these risks are associated with oral pills. However, cases of mild headaches or dizziness should be reported to the doctor.
- They provide you with protection for 2 to 3 months. There is no need to use any other form of contraception during this period.
B. Other non-contraceptive benefits
- May decrease menstrual cramps.
- May decrease menstrual bleeding.
- May improve anemia.
- Protects against some causes of pelvic inflammatory diseases.
- Decreases chances of ectopic pregnancy.
- Decreases benign breast disease.
- Protects against endometrial cancer.
- Any nurse or trained non-medical staff can administer the injection. There is no need to book an appointment with your gynaec every time you need a shot.
DISADVANTAGES
- Menstrual Irregularities - Spotting, breakthrough bleeding and sometimes skipping of your periods are the side effects of these contraceptives. However, skipping of your periods is natural when you are on the IC and it does not cause any harm… and, of course, it helps in cases of anemia!
- Planning or postponement of the period is not possible when the woman is on ICs.
- One cannot accurately predict the timing of the period, which may create a slight problem, especially when planning a holiday or even religious function.
- There may be a delay in return to fertility after discontinuing ICs. Pregnancy may not occur immediately. On an average it takes 2-3 months after you stop taking the pill or removing a Copper T to resume fertility. If you are using injectable contraception, this period is longer, and can be 4 to 5 months.
- ICs do not provide protection against STDs or HIV. Neither do oral pills for that matter. Only condoms or any other barrier method of contraception can provide this protection.